Patients are getting lost between the in-patient and out-patient world. This results in higher readmissions, sicker patients, and skyrocketing healthcare costs.
Today, on average, the national rate for 30-day all-cause readmission is almost 15% (see Figure 1 below).
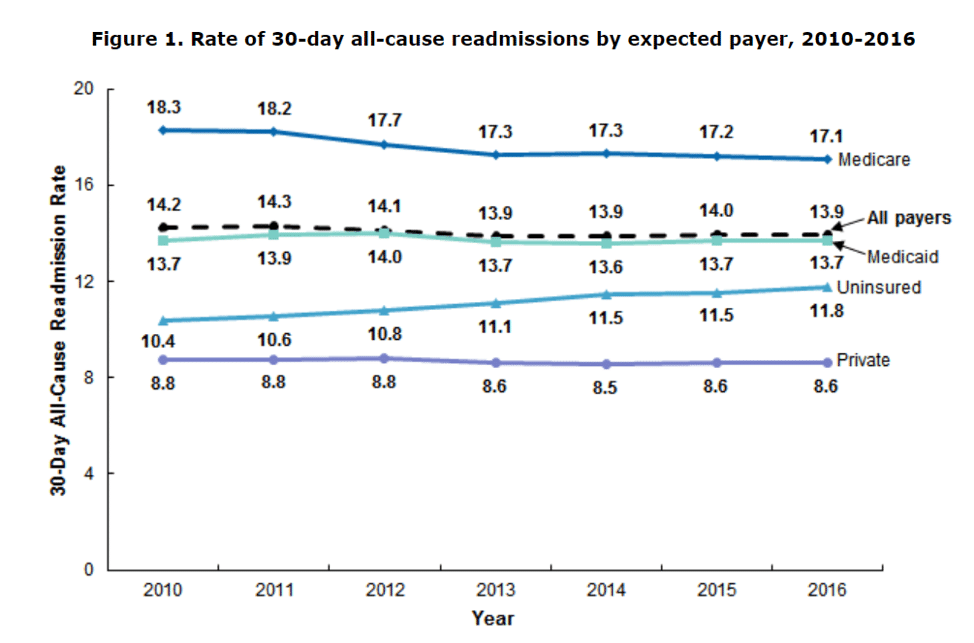
Source: Agency for Healthcare Research and Quality (AHRQ), Center for Delivery, Organization, and Markets, Healthcare Cost and Utilization Project (HCUP), 2010-2016 Nationwide Readmissions Database (NRD)
Patients who return to the hospital following discharge are costly and risky, but more importantly AVOIDABLE.
According to America’s Health Ranking Senior Report, the top 3 reasons patients return to the hospital after a short time after discharge are:
- Confusion about how and when prescribed medications should be taken
- Miscommunication by hospital staff of important information, such as test results, to the patient’s primary care providers
- Improper follow-up care after discharge without adequate instruction (patients and family members may not understand how to provide proper care at home)
Hospitalists are physicians, primarily internal medicine or family medicine specialists, who round on patients during their stay in the hospital. This specialty emerged out of the unsustainable model of your family doctor seeing you in the out-patient world and then rounding on their patients in the evening and on weekends if they were hospitalized. Obviously, this results in the patients being cared for by physicians who are unfamiliar with their medical history. This would be way less of a concern or problem if the Hospitalist could have access to the patient’s complete medical history.
In a recent blog I authored, entitled Overcoming the Complexity of Interoperability, I wrote about the disconnect this presents for all providers caring for patients in both settings—the hospital and the out-patient clinic. Most often, the hospital EHR does not link or share information with the out-patient provider. So, when a patient is discharged from the hospital, the primary care physician is likely unaware of the hospitalization and often, doesn’t receive a summary of the hospitalized stay.
11 percent of hospital readmissions are directly related to non-adherence to medication recommendations
When a patient is discharged from the hospital, they receive instructions to assist them with how to manage their own care at home. Patients will receive a summarized list of what medications they need to take, including why, when, how, and any possible side effects that may occur with each medication. They also receive recommendations to make a follow-up appointment with their primary care doctor—and may receive multiple specialty follow-up appointment recommendations depending on their illness and needs.
Additionally, they may require tests, procedures, and lab work. Often, patients do not easily understand these instructions and do not adhere to the follow-up instructions provided for them.
Approximately 17% of elderly patients discharged from the hospital are readmitted within 30 days
Add in our aging, underserved and those with cognitive impairment population, and the risk for readmission increases. Additionally, when a patient has multiple comorbidities and more complex health issues, the out-patient follow-through is crucial, and demands for a comprehensive discharge management process.
DO THESE 6 THINGS NOW TO DECREASE YOUR HOSPITAL READMISSION RATE:
- Aim for a 100 percent benchmark rate of influenza immunization
- Identify your top 5 readmission diagnoses, and develop a very specific comprehensive plan for discharge for each diagnosis
- Standardize your discharge instructions across your system of care for continuity and preciseness
- Provide thorough medication reconciliation and education, and ask the patient to repeat what the instructions are to ensure understanding
- Begin a discharge phone call program (either internally or contract from a professional call center such as Dedicated Resource Scheduling to check in with the patient
- Provide discharge appointments at the bedside BEFORE THE PATIENT LEAVES THE HOSPITAL
#6 Begs the question: How do I accomplish that?!
THERE’S AN APP FOR THAT!
Meet EVOLVE by HybridChart – Our fourth generation software platform.
Take control of your entire workflow through a user-friendly solution created by a physician. Medical software too often fails to address the specific needs of providers. Rounding at one or more hospitals presents a unique challenge. There is the need for effective team collaboration and easy charge capture. Census management means true collaboration among provider and staff. Rounding at multiple facilities just got way easier. Covering on-call now has the luxury of essential information for clean hand-offs. Charge capture takes less than five seconds. Diagnoses are easy to find and follow the patient. Customized charge menus make it easy to enter the correct charge. Don’t let billing for your work slow you down. Charge in real-time and focus on caring for the patient.
HybridChart has numerous levels of safeguards against missed charges. The Charge Checker feature will scan every day of an admission and assure there are charges. Using the Charge Matrix you have visibility of all charges from multiple providers per day for any given patient.
Most practices see a revenue increase of 8-10% after using HybridChart – attributed to capturing every charge for every patient. Charges are complex enough with just the diagnosis codes and charge codes. To make your charges accurate HybridChart allows you to easily adjust the Date of Service and assign Secondary Billers such as nurse-practitioners and physician assistants. Modifiers can be built into specific Billing Modules or choose from a customized list managed by your practice. Seamlessly navigate our Charge Capture workflow and save time without losing accuracy.
An automated charge capture system may be the most profitable investment that you can make in your practice today.
You can instantly boost your revenue by 10% using our modern, high-tech and easy-to-implement charge capture system.
Smarter Rounding and Workflow Software for Doctors
At HybridChart, we provide technology that connects your healthcare team, increases efficiencies, AND improves your bottom line. HybridChart’s cloud-based software adapts to your practice’s unique workflow and will improve your profitability and patient outcomes by utilizing our 5 features: census management, charge capture, secure messaging, discharge management, and data analytics.
NEVER miss another charge and get PAID for the work you do!
If you are interested in taking your medical practice to the next level and want to employ the best hospital charge capture practice available in the industry, come visit our website at www.hybridchart.com, or call us at 1-877-684-0608 for a demo today!





